
Health is a crown on the heads of the healthy that only the sick can see.

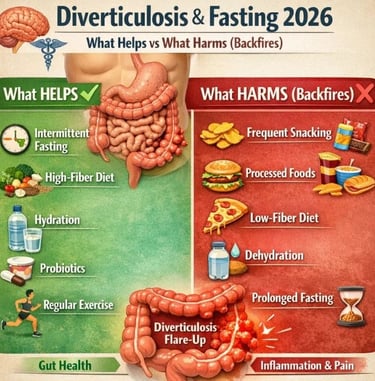
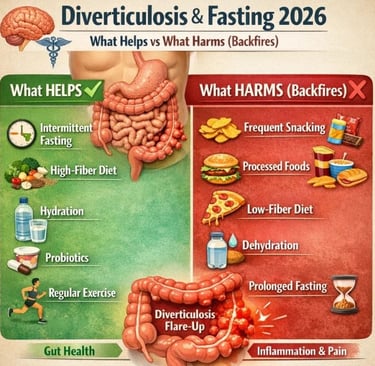
⚕️🧠 Diverticulosis & Fasting 2026: What Helps vs What Harms (Backfires)
Fasting with diverticulosis: helpful or harmful? Learn what works, what backfires, and how to protect your gut safely.
FASTINGGASTROINTESTINAL
Dr Hassan Al Warraqi
4/20/20269 min read

⚕️🧠 Diverticulosis & Fasting 2026: What Helps vs What Harms (Backfires)
Fasting with diverticulosis: helpful or harmful? Learn what works, what backfires, and how to protect your gut safely.
A comprehensive, evidence-based guide covering intermittent fasting, bowel rest during flares, dietary phases, and long-term prevention strategies for diverticular disease.
Introduction
Diverticulosis is one of the most common conditions affecting the digestive tract, particularly in adults over 50.
It is characterized by the presence of small, bulging pouches — called diverticula — that form in weak spots along the colon wall.
While many people live with diverticulosis for years without any symptoms, it carries the risk of progressing to diverticulitis, an active and often painful inflammatory state.
In recent years, fasting has gained significant popularity as a health and longevity strategy.
Naturally, people with diverticular disease have begun to ask:
Is fasting safe for me? Can it help or hurt?
The answer is nuanced and depends critically on your current state — whether you're in a stable, asymptomatic phase or experiencing an active flare.
This guide breaks it all down clearly.
Important: This article is for informational purposes only and is not a substitute for professional medical advice.
Always consult your gastroenterologist before making significant dietary changes.
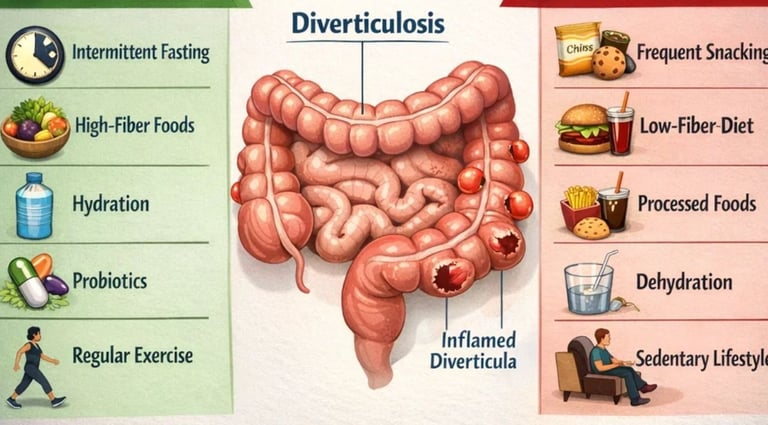
Understanding the Condition: Diverticulosis vs. Diverticulitis
These two terms are frequently confused, but the distinction is critical for understanding how fasting applies to your situation.
Structural condition
Diverticulosis
Small pouches (diverticula) form in the colon wall. Usually silent — most people don't know they have it.
Goal: prevention.
Active inflammation
Diverticulitis
Those pouches become inflamed or infected, causing pain, fever, nausea, and altered bowel habits.
Requires medical treatment.
Diverticulosis itself does not cause symptoms in most people.
The primary long-term management goal is to prevent it from ever progressing to diverticulitis.
Diet — particularly fiber intake and hydration — is the cornerstone of that prevention.
How Diverticula Form : The Pressure Problem
Understanding the mechanics of diverticula formation helps explain why diet and fasting decisions matter so much.
When stools are hard and slow-moving, the colon must generate significantly higher internal pressures to move them through.
Over time, this elevated intracolonic pressure forces weak points in the colon wall to bulge outward, forming pouches.
The single most effective protection against this process is maintaining soft, regular stools through a high-fiber, well-hydrated diet.
Anything that consistently contributes to constipation or dehydration — including poorly managed fasting — works against that goal.
Fasting and Diverticulosis: Two Very Different Scenarios
Scenario 1: Therapeutic bowel rest during an acute flare
If you are experiencing active diverticulitis — characterized by lower abdominal pain, fever, nausea, or significant changes in bowel habits — a prescribed period of bowel rest is often part of the standard treatment protocol.
This is not voluntary fasting; it is a medically directed intervention.
For uncomplicated diverticulitis, physicians typically recommend a clear liquid diet for two to three days, or until symptoms improve.
In more severe or complicated cases, patients may be advised to take nothing by mouth at all until the acute inflammation subsides.
Clear liquids generally include: water, sparkling water, unsweetened tea, black coffee, clear consommé, and bone broth.
Some providers allow pulp-free juice or gelatin.
Fluids with added sugar or artificial sweeteners may be advised against by some practitioners.
Once symptoms improve, the diet is gradually advanced — first to low-fiber foods, then slowly back toward a regular high-fiber diet over the following weeks.
Critical warning: If you suspect you are having a diverticulitis attack, seek medical attention promptly.
The clear-liquid phase is only appropriate under medical supervision for a short, defined period.
Scenario 2: Intermittent fasting with stable, asymptomatic diverticulosis
For individuals with diverticulosis who are currently symptom-free, the question of fasting is more nuanced.
There is currently no robust clinical evidence specifically studying fasting in people with diverticulosis.
However, the general principles of what helps and harms the condition can guide a sensible approach.
Short, well-managed fasting windows — such as a 12–14 hour overnight fast — are generally unlikely to cause harm if fiber and hydration targets are consistently met during eating windows.
The concern arises with longer or more restrictive fasting patterns that reduce overall fiber intake, promote dehydration, or lead to irregular bowel habits.
Potential Benefits of Fasting (When Done Carefully)
Temporary gut rest: Fasting periods reduce the mechanical load on the digestive tract, which may allow mild, subclinical inflammation to settle.
Reduced intracolonic pressure: When the colon is not actively processing food, internal pressures drop — which is fundamentally protective for people with diverticula.
Metabolic improvements: fasting has documented benefits for insulin sensitivity, inflammation markers, and metabolic health broadly — all of which have indirect protective effects on the gut.
Autophagy: Extended fasting (typically beyond 16 hours) triggers cellular autophagy, a process of cellular cleanup that may reduce low-grade systemic inflammation over time.
Risks and Ways Fasting Can Backfire
The risks of fasting with diverticulosis are not trivial and represent exactly the mechanisms that worsen the condition:
Constipation: Reduced food volume during fasting means reduced stool bulk and slower motility.
⚠️ Warning: Prolonged use of a clear liquid diet can cause nutrient deficiencies.
Never extend bowel rest beyond what your doctor recommends
This directly increases intracolonic pressure — the primary driver of diverticula complications.
Dehydration: People who fast often unintentionally reduce their fluid intake.
Dehydration hardens stools, compounding the constipation risk.
Reduced fiber intake: If fasting compresses the eating window significantly, hitting adequate daily fiber targets (25–38g) becomes harder, undermining the primary long-term protection strategy.
Gut microbiome disruption: Prolonged or aggressive fasting may alter gut bacterial composition in ways that are not well understood in the context of diverticular disease.
Refeeding risk: Breaking a long fast with low-fiber, processed, or high-fat foods is arguably worse than not fasting at all — it can cause an abrupt shift in bowel function that stresses an already vulnerable colon.
When to avoid fasting entirely: Do not fast (or only do so under direct medical supervision)
if you have active diverticulitis, a history of frequent flares, chronic constipation, or recent unexplained abdominal pain.
Anti‑inflammatory effects: Prolonged fasting (≥16 hours) triggers autophagy, a cellular cleanup process that may reduce low‑grade gut inflammation.
Busting Common Myths
Myth
Fasting heals or reverses diverticulosis.
Fact
Fasting cannot remove existing diverticula.
It may help manage symptoms but does not reverse the structural condition.
Myth
Nuts, seeds, and popcorn must be avoided forever.
Fact
Current guidelines confirm these foods are safe outside of flares and may even be protective due to their fiber content.
Myth
A prescribed clear liquid diet during a flare is the same as intermittent fasting.
Fact
These are fundamentally different.
One is a short-term medical intervention; the other is an elective lifestyle dietary pattern.
Myth
More fiber is always better, even without water.
Fact
Fiber without adequate hydration can worsen constipation.
Water is essential for fiber to function properly in the colon.
Dietary Phases: A Complete Framework
Acute flare
2–3 days, doctor-prescribed Bowel rest; allow inflammation to subside Water, clear broth, pulp-free juice, gelatin, popsicles, unsweetened tea All solid foods and high-fiber items
Recovery
Days to weeks Gradually reintroduce foods without stressing the bowel White rice, white bread, eggs, poultry, fish, peeled/cooked vegetables Raw vegetables, whole grains, nuts, seeds, high-fiber foods
Maintenance
Lifelong approach Prevent new diverticula; reduce flare risk Vegetables, fruits, whole grains, legumes, beans, plenty of water (6–8 glasses/day)
Consistently low-fiber diets, excessive red meat, ultra-processed foods
The Smarter Approach: What Actually Protects the Colon
Rather than relying on fasting as a primary strategy, the evidence points consistently to three pillars that genuinely reduce risk:
Pillar 1
Fiber (25–38g daily)
Softens stool, reduces intracolonic pressure. Whole grains, legumes, vegetables, and fruit are your best long-term tools.
Pillar 2
Hydration (6–8 glasses/day)
Fiber needs water to work. Dehydration turns fiber into a constipation risk rather than a remedy. This is especially critical during any fasting period.
Pillar 3
Physical movement
Regular exercise improves bowel motility and reduces colon transit time — directly lowering pressure buildup risk.
If fasting
Keep it moderate
A 12–14 hour overnight fast is the safest pattern.
Avoid 24+ hour fasts without medical guidance. Always break fasts with fiber-rich foods and fluids.
Medical Guideline Landscape
It is worth noting that formal clinical guidelines on intermittent fasting specifically for diverticulosis are limited.
The American Gastroenterological Association (AGA) and the American College of Gastroenterology (ACG) focus their guidance primarily on the management of acute diverticulitis episodes — recommending bowel rest and a clear liquid diet during active flares.
Neither organization currently provides specific endorsements or contraindications for elective fasting in stable diverticulosis.
This gap in the guidelines reflects a genuine gap in research, not a tacit endorsement.
Individuals with diverticular disease should treat this uncertainty with appropriate caution and always loop in their healthcare provider before adopting any fasting protocol.
Special Considerations
Ramadan fasting and diverticulosis
Extended daily fasting periods, such as those observed during Ramadan, present specific challenges.
The long fasting window, combined with reduced overall hydration during daylight hours, requires careful planning.
Prioritizing water and high-fiber foods during Suhoor (pre-dawn meal) and Iftar (breaking fast) is essential.
Recent GI guidelines on Ramadan fasting classify stable diverticulosis as lower risk compared to active diverticulitis, but individual assessment with a physician is still strongly recommended.
Conclusion
Diverticulosis and fasting can coexist, but only when the condition is stable and the fasting approach is moderate and well‑planned.
For acute diverticulitis, medically supervised bowel rest with a clear liquid diet is standard care—but this is not the same as voluntary intermittent fasting.
Coexisting conditions
If you have diabetes, kidney disease, or are on medications that require food timing, fasting carries additional complexity.
Medication schedules and blood sugar management may need to be adjusted around any fasting window.
This is a conversation that must happen with your treating physician before any fasting begins.
Frequently Asked Questions
Can intermittent fasting trigger a diverticulitis flare?
Indirectly, yes — if fasting leads to constipation, dehydration, or reduced fiber intake, these outcomes can increase intracolonic pressure and potentially trigger inflammation.
Fasting itself is not the direct cause, but its consequences can be if it is not well managed.
What is the safest fasting window for someone with diverticulosis?
A 12–14 hour overnight fast is generally considered the most manageable pattern, as much of it occurs during sleep.
This minimizes disruption to eating patterns while still delivering some of the metabolic benefits of time-restricted eating.
Should I take fiber supplements during a fasting window?
Soluble fiber supplements (like psyllium husk) are typically safe to take with water during a fasting window and may actually support motility.
However, discuss this with your doctor, especially if your fasting goal involves metabolic benefits that require a truly clean fast.
Is bone broth a good option during a flare?
Yes. Clear bone broth is generally listed among the accepted clear liquids during acute diverticulitis bowel rest.
It provides some electrolytes and a small amount of protein while being easy on the digestive tract.
How do I break a fast safely with diverticulosis?
Start with something hydrating and easy to digest — a small serving of oatmeal, fruit, or a vegetable-based soup works well.
Avoid breaking a fast with red meat, fried foods, or very low-fiber options. Rehydrate first, then eat.
Can intermittent fasting cause diverticulitis?
There is no evidence that intermittent fasting causes diverticulitis. However, if fasting leads to chronic constipation or dehydration, it could theoretically increase the risk of a flare‑up in someone who already has diverticulosis.
Is a clear liquid diet the same as fasting?
No. A clear liquid diet provides some calories and hydration, whereas true fasting involves zero calorie intake. For acute diverticulitis, a clear liquid diet is preferred over complete fasting because it maintains hydration and electrolyte balance.
Can I fast during Ramadan if I have diverticulosis?
Many Muslims with stable, asymptomatic diverticulosis can safely observe Ramadan fasting (dawn to dusk).
However, the key is what you eat during non‑fasting hours—prioritize high‑fiber foods, fruits, vegetables, and plenty of water. If you have a history of recurrent diverticulitis or are currently symptomatic, consult an imam and your doctor for a religious exemption.
What should I eat to break a fast safely with diverticulosis?
Break your fast with water and a small, fiber‑rich meal. Examples:
A bowl of oatmeal with berries
Whole‑grain toast with avocado
Lentil soup with vegetables
A smoothie made with spinach, banana, and flaxseed (ground)
Avoid large, greasy, or highly processed meals.
How long after a diverticulitis attack can I try intermittent fasting?
Wait until you have fully recovered and have been cleared by your doctor.
Typically, this means you have successfully transitioned back to a high‑fiber diet without any abdominal pain or bowel changes for at least 2–4 weeks.
Can I take fiber supplements while fasting?
Fiber supplements (e.g., psyllium husk) are best taken with food and plenty of water. If you are following an intermittent fasting schedule, take your fiber supplement during your eating window. Never take dry fiber supplements without water.
The bottom line
Fasting is not a treatment for diverticulosis and cannot reverse the structural changes in the colon.
Short, well-managed intermittent fasting can be neutral or mildly beneficial for stable diverticulosis — but it becomes counterproductive the moment it causes constipation, dehydration, or reduced fiber intake.
The evidence-based foundation remains: fiber + hydration + movement over extreme fasting
=============================================================================================================================================================================================
⚕️🧠 Diverticulosis & Fasting 2026: What Helps vs What Harms (Backfires)
https://www.h-k-e-m.com/-diverticulosis-and-fasting-2026-what-helps-vs-what-harms-backfires
diverticulosis fasting, diverticulitis diet, intermittent fasting gut health, colon health fiber, diverticulosis treatment diet, fasting and inflammation gut, bowel rest diverticulitis, high fiber diet colon health, fasting risks constipation, gut health tips
🔖 Hashtags
#Diverticulosis #Diverticulitis #GutHealth #FastingScience #IntermittentFasting #DigestiveHealth #HighFiberDiet #ColonHealth #Inflammation #HealthyGut #NutritionScience #MedicalInfo #FastingRisks #MetabolicHealth #Wellness2026
⚡ High-Impact Hooks
⚡ Fasting isn’t always healing… sometimes it harms
🚨 The mistake that silently increases colon pressure
🧠 Gut rest ≠ starving your gut
⚖️ The balance most people miss
🥗 Fiber still beats extreme fasting
===========================================================================================================================================================================================================================================
🧠🫀 Neurocardiology & Fasting: Unlocking the Heart–Brain Connection (In Short)
Fasting can shift your autonomic nervous system toward a calmer, more balanced state.
It may activate the vagus nerve, improve heart rate variability (HRV), and reduce stress-related inflammation.
Bottom line:
Fasting doesn’t just affect metabolism—it helps regulate how your brain and heart communicate.
===============================================================================================================================================================================================================================================





Get in touch
Address
Cairo Al Rehab
Contacts
+20 109 405 2056
hassanalwarraqi@h-k-e-m.com
